Feature
SCN2A Q&A with Professor Stephan Sanders
February 23, 2024

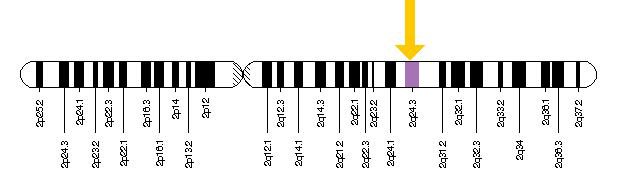
DNA changes in the SCN2A gene cause a range of neurological conditions, affecting hundreds of thousands of people globally. As SCN2A is located at position 24.3 on the long arm of chromosome 2, February 24th (2/24) was chosen as International SCN2A Awareness Day.
Professor Sanders specialises in the genetics of neurodevelopmental disorders, including genomics, functional genomics, and therapeutics. His lab’s research has helped further our understanding of the role of SCN2A mutations in human disorders.
What is SCN2A?
The SCN2A gene encodes a sodium channel called NaV1.2. Found in neurons, it plays a key role in the cell’s ability to generate and transmit electrical signals necessary for brain function and for learning.
The NaV1.2 channel sits at the surface of the cell and forms a pore, which can open to allow sodium to pass into the cell. It is called a voltage-gated sodium channel because it opens in response to changes in voltage, a kind of electrical “signal.”
The channel’s protein structure, comprised of four domains, includes special amino acids that make up the “Ion Selectivity filter,” which allows only sodium to pass through. For this to work, it is critical that these amino acids are held in the right positions.
Mutations in the SCN2A gene can alter the structure and function of the NaV1.2 channel, leading to disorders including epilepsy, autism, and developmental delay.
What are the SCN2A-related disorders?
Pathogenic variants in SCN2A can cause a range of neurodevelopmental disorders. SCN2A dysfunction has been associated with three disorders or symptom groups:
Benign infantile familial seizures (BIFS or BFNIS): Seizures begin before 12 months of age and resolve by 2 years of age. There are no long-term developmental or neurological issues.
Epileptic encephalopathy (EE): Seizure onset before 12 months of age, often reported before birth, continues beyond 2 years of age. The condition is characterised by developmental delay, often severe.
Autism Spectrum Disorder (ASD) and/or Developmental Delay (DD): No seizures before 12 months of age, delayed developmental milestones. ASD is often on the low-functioning or severe end of the spectrum. Patients may have late onset (>12 months) seizures, which are common in ASD and DD.
SCN2A research at the Sanders Group
The Sanders Lab continues to prioritise research aimed at understanding the role of SCN2A in human disorders and developing therapies. They have taken two approaches to understanding the role of neurodevelopmental disorder genes: 1) looking at genes related to neurodevelopmental disorders en masse to identify patterns that can help identify a specific cell type and 2) investigating the genes with the strongest relationship to neurodevelopmental disorders, such as SCN2A, in-depth.
Through the first approach, the Sanders Lab has helped delineate two major functional roles of genes associated with ASD and neurodevelopmental disorders: gene expression regulation and neuronal communication (the latter of which is the role of the SCN2A gene). They have also shown that these genes appear to act through excitatory neurons in the brain.
The second approach has focused mainly on SCN2A and is performed in collaboration with the Bender lab at UCSF, the SCN2A family group, and Simons VIP. By integrating genetic data across multiple cases and groups of patients with structural data on the NaV1.2 protein encoded by SCN2A and electrophysiology, they demonstrated that loss-of-function mutations of SCN2A lead to ASD and developmental delay, while gain-of-function mutations lead to epileptic encephalopathy.
More recently, the Sanders Lab has expanded to the University of Oxford and has developed projects and partnerships geared toward developing therapeutics, like antisense oligonucleotides (ASOs), for neurodevelopmental disorders and genes like SCN2A. They hope that by prioritising genes with more straightforward pathophysiologies for ASOs as proof of concept, they can soon expand these methodologies to other more complex neurodevelopmental disorder genes.
SCN2A case study

Tischa Jenkinson, a parent of a child with an SCN2A-related condition, shares her experience:
My son has SCN2A and is currently twelve years old. It is a debilitating condition that affects him in many ways, including having epilepsy and autism. We discovered he had SCN2A when he was two years old. At that point, there were only forty diagnosed cases. It was totally unknown to many doctors, and as a family, we had so many questions and no answers.
A decade on, the work Stephan has been doing is potentially life-changing. Any therapy that can help improve his cognition will make the difference between him being able to work, have better relationships and be safer as he goes into adulthood. Even if it is only a small difference, that difference to him is profound.
For my son, it's key that the therapies are developed quickly, and this team is committed and working tirelessly to develop the therapies that can help him.
Tischa’s commitment to fighting the condition led her to join the SCN2A Family Foundation as a marketing director in 2023. The foundation is the world’s largest SCN2A community and aims to accelerate research that can improve the lives of those affected by SCN2A-related disorders around the world.
In numbers around the world, we hope to find therapies and share support for all children with SCN2A. My son is a warrior. Fighting over 3000 seizures in a year and surpassing all medical odds, he walks, talks and enjoys his life more than anyone I know. With the work of Stephan and his team, we feel positive for an even brighter future for him as he becomes a teenager.
How can one gene cause three different disorders?
The work of the Sanders and Bender Labs has shown that there are two main ways the gene can be disrupted: Gain of Function (GoF) or Loss of Function (LoF) of the sodium channel.
Mild gain-of-function variants typically lead to Benign infantile familial seizures. These variants are often inherited, so the seizures can run in families. Around one year of age, the seizures stop, and the child develops typically.
Severe gain-of-function variants lead to early onset epileptic encephalopathy, with severe seizures that persist after the age of one year and intellectual disability.
A loss-of-function variant reduces the excitability of the channel or destroys its function altogether. This loss of function is associated with autism spectrum disorder and/or intellectual disability without seizures, though sometimes seizures occur in childhood.
Recently, scientists have identified a fourth pattern in which variants fall in the middle of that scale, leading to a mixture of both gain and loss-of-function at the same time. These individuals often have seizures that begin around 6 to 12 months, which can be difficult to treat and associated with longer-term intellectual disability.
What are the latest therapeutic strategies, and how far have they come?
Therapeutic strategies have historically been aimed at easing symptom burden, for example, using anti-seizure medications. These “small molecule” drugs often come with systemic and unwanted side effects, so research efforts continue to focus on improving the efficacy and selectivity of anti-epileptic medications. Clinical trials for new variations of drugs that are more specific, PRAX-562 and PRAX-628, for example, are currently underway.
Recently, a gene-specific ASO called elsunersen (PRAX-222) has demonstrated a significant, dose-dependent reduction in seizures and improvement in behavioural and locomotor symptoms in the early stages of clinical trials. It has the potential to be the first disease-specific treatment for gain of function SCN2A epileptic encephalopathy, having received Orphan Drug Designation (ODD) and Rare Pediatric Disease Designation (RPD) from the FDA.
What are the future prospects for treatments of SCN2A-related disorders?
With the advent of genomic medicine and new therapeutic modalities like antisense oligonucleotides (ASOs), we are in a promising time for rare disease research and treatment. ASOs administered at critical developmental time points may prove to be an optimal treatment for many SCN2A-related disorders. Another approach developed by the Ahituv Lab in San Francisco is showing promise for loss-of-function cases, using CRISPR technology to ‘activate’ the unaffected allele and replace the non-functional one. Ultimately, CRISPR gene editing may allow variants to be corrected directly in the brain.
We will strive, however, for a future where all individuals have appropriate and effective treatments and can live a life unhindered by SCN2A-related disorders.
Useful Links
Sanders, Stephan J et al. “Progress in Understanding and Treating SCN2A-Mediated Disorders.” Trends in neurosciences vol. 41,7 (2018): 442-456. doi:10.1016/j.tins.2018.03.011
Ben-Shalom R, Keeshen CM, Berrios KN, An JY, Sanders SJ, Bender KJ. Opposing Effects on NaV1.2 Function Underlie Differences Between SCN2A Variants Observed in Individuals With Autism Spectrum Disorder or Infantile Seizures. Biol Psychiatry. 2017;82(3):224-232. doi:10.1016/j.biopsych.2017.01.009